If you wear contact lenses, a good eye care regime can help prevent eye infections. An infection can cause symptoms like blurred vision or dry eyes. We’ve put together this handy guide on avoiding and treating eye infections for contact lens wearers. You can also call us for free advice on contact lenses, or ask our optician about eye care. We’re available Monday - Friday 8:00 - 21:00, and Saturday - Sunday 8:00 - 18:00 on 020 7768 5000, or by emailing help@visiondirect.co.uk.
Free delivery for orders £59 and up
Free delivery for orders £59 and up
Contact Lenses and Eye Infections
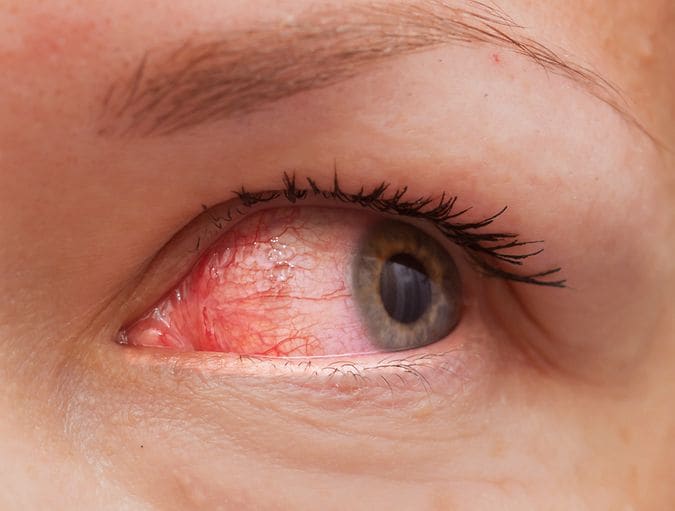
Because you are inserting something into your eye using your finger, wearing contact lenses can make you more susceptible to an eye infection; this is easily avoided if you look after your lenses well and always wash your hands before putting in your contact lenses.
Infections can occur within different parts of your eye, including your eyeball, the inside of your eyelid or your cornea. Here’s what to look out for and how to avoid them.
• Pain or swelling
• Redness of the eye
• Itching
• Discharge of a yellow or creamy mucus
• Blurred vision
• Dry eyes
• Watery eyes
• Sensitivity to light
In the event that you experience any of these symptoms, you should consult your general practitioner or optician at the earliest opportunity so that the condition may be diagnosed and appropriate treatment provided, which may include a prescription for medication. It is important not to attempt to diagnose an infection yourself as failure to obtain the most appropriate treatment may prolong the infection and could result in long-term damage to your vision.
Also, it may be necessary for your GP or optician send a sample from your eye for culturing in order to identify the infection from which you are suffering. This is the case when a particular antibiotic is needed to treat the infection. An attempted self-treatment might result in you obtaining a broad-spectrum or generic over-the-counter medication which is ineffective in tackling your infection.
If you experience the symptoms of an eye infection and normally wear contact lenses, it is advisable to remove them and wear your glasses until you have consulted your GP or optician. You will be advised whether you should continue to refrain from wearing your lenses and at which point you may resume their use. For more information on this topic, please see our page on conjunctivitis and contact lenses.
Undoubtedly eye infections are often unpleasant and to be avoided where possible as they may inhibit your daily life and activities such as driving or working on a computer.
The most sensible preventative action you can take is to avoid close contact with a person who you know to have an eye infection. Some infections, such as conjunctivitis, are highly infectious (the Health Protection Agency advises that children with conjunctivitis are to be excluded from school or nursery in the event of an outbreak). If you are in contact with someone who is known to be suffering with an eye infection of any type, thorough hand washing and sanitising using antibacterial gels is recommended. It is also important that the affected individual regularly washes his or her hands.
Washing bed linen and towels that a sufferer has used is important to restrict the spread of an infection within the home.
For contact lens wearers, keeping your lenses clean is extremely important to help to prevent eye infections. You should practise high standards of hand hygiene and only insert lenses into your eyes that you are confident are clean. Wearing contacts while you sleep can also contribute to eye infections so remove them at night before you retreat to bed.
Prompt diagnosis and treatment of an eye infection usually results in it clearing up rapidly, especially if the infection is caused by bacteria as it will respond effectively to antibiotic eye drops.
A viral infection is harder to treat and you may be prescribed medication to help to relieve the discomfort initially while the infection resolves by itself. More serious viral infections may be treated with antiviral eye drops while steroids can be a valuable way to reduce inflammation in the tissue surrounding the eye.
Many treatments are supplied in the form of drops which are applied directly to the eye while in some instances your GP or optician may prescribe oral medicines. It is important to follow the dosage instructions carefully and, in the event that the infection shows little sign of improving, that you consult your GP or optician again.
A wide variety of eye infections exist which are caused by different bacteria, viruses or fungi:
• Conjuctivitis: A common and highly contagious infection (also known as 'red eye'), conjunctivitis is often prevalent in schools, nurseries and other locations where large numbers of children mix. It is characterised by the inflammation of the conjunctiva, the thin tissue layer which covers the front of the eye. Symptoms include redness, itching and a yellow discharge (which may be worse when waking from sleep). The cause may be a bacterial or viral infection or an allergic reaction to pollen or substances such as shampoo.
• Viral Keratitis: (inflammation of the cornea): A variety of other viral infections can cause symptoms which bear a similarity to conjunctivitis, such as the herpes simplex virus or adenovirus.
• Fungal Keratitis: Fungal eye infections are associated with the Fusarium fungi which is commonly found in organic substances. Being poked in the eye by a tree branch, for example, can transfer the fungus to a person's eye where it can reside causing infection, the symptoms of which include pain, redness, discharge and blurred vision.
• Acanthamoeba Keratitis: Although less common, the Acanthamoeba Keratitis infection can be potentially serious and threaten to cause long-term damage to a sufferer's eyesight. Often caused by a parasite which enters the eye, contact lens wearers are more prone to this infection if good standards of hygiene are not observed and safety tips, such as not wearing lenses while swimming, are not followed.
• Endophthalmitis: Most eye infections are superficial and affect only the exterior tissue of the eye but in some cases a more serious infection may penetrate the eye, the outcome of which can be serious. An injury to the eye and, in rare cases, a complication of cataract treatment, endophthalmitis requires urgent antibiotic treatment. Initial symptoms may include a loss or worsening of vision, pain, redness and swelling. As the infection progresses, symptoms - which may occur more mildly - include blurred vision, eye pain and sensitivity to light.
• Trachoma: Less common in developed countries, trachoma is a leading cause of blindness in many undeveloped areas of the world and travelers should be aware of the potential for infection which is spread by flies in places where sanitation is poor. Trachoma causes scarring to the inner eyelids which in turn leads to the eyelids turning in on themselves; the contact between the eyelashes and the sensitive tissue of the cornea may cause irreparable damage, with blindness a common consequence.
An infection that penetrates the exterior of the eye can lead to more serious complications including a stye, blockage of the tear ducts, ulcers of the cornea, orbital cellulitis, deterioration of vision and blindness.
While serious complications are less common, any suspected infection of the eye should be assessed as a matter of urgency by a medical professional so that you can receive the appropriate treatment as soon as possible.
